A disease of high-producing dairy cows occurring soon after calving. It is also called postparturient hemoglobinuria and is characterized by intravascular hemolysis, hemoglobinuria, and anemia.
Table of Contents
Etiology
a. Ration low in P, hay and grass from low P area, draught
b. Cu deficiency (incidence reduced when supplemented)
Precipitating factor
b. Grazing Brassica sp. plants, rape and turnip and other cruciferous plants, a large quantity of beet pulp, sugar cane top (low in p).
a. Exposure to cold weather, cold water – erythrocytes becomes more sensitive to hemolysis when there is hypophosphatemia & hypocupremia
Epidemiology
- Prolonged hypophosphatemia is an important predisposing factor
- ‘P’ deficient soil and drought condition act as precipitating factors
- 50% mortality and 40% morbidity
- Adult cow & she buffalo 3-6 weeks after delivery are more prone.
- Animals in 3-6th Lactation are more prone
- Geographical distribution: Throughout the world including India
- In India: It is very common in North India – Punjab, Haryana, M.P, Rajasthan, Western part of Maharashtra.
- In Europe & North America the diseases is more common during a prolonged period of housing.
Pathogenesis of postparturient hemoglobinuria
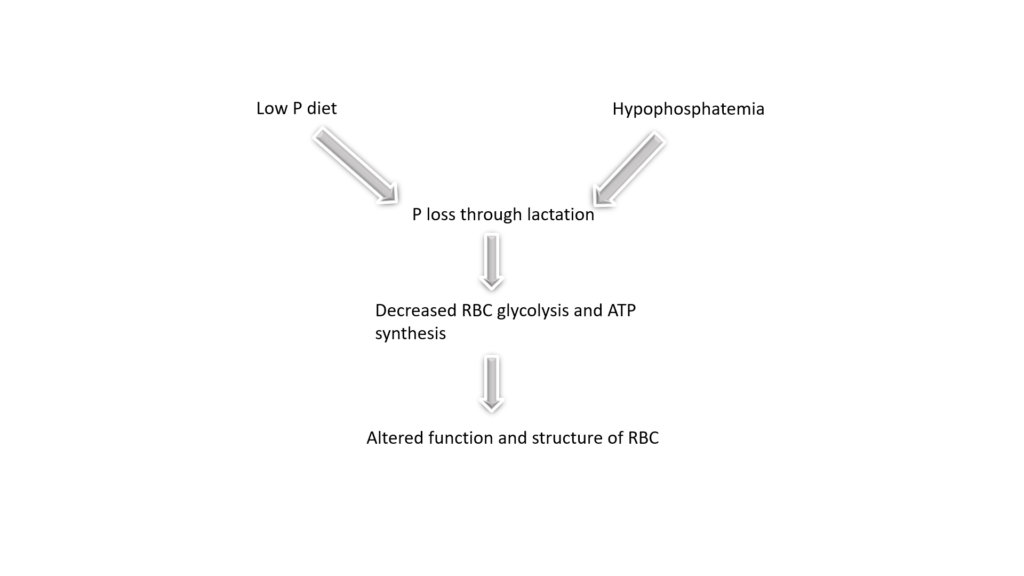
• Haemoglobinuria and hemolysis do not occur always. Death is mainly due to anemic anoxia.
• The possible role of Cu and Se deficiency in hypophosphatemia is unclear. In cases of Cu deficiency, there will be microcytic hypochromic anemia.
• Cu and Se provide protection against effects of orally acquired hemolytic agents of cruciferous
plants.
Clinical signs
Acute cases
• Rapid onset after 2-4 weeks of calving, the course is 3-5 days, red-colored urine, anorexia, weakness, severe depression of milk yield.
Less acute cases
- Eats and gives milk for 24 hours after red-colored urine.
- Dehydration occurs quickly.
- Haemoglobinuria, inappetence, severe depression of milk yield.
- Heart rate is increased and bounding.
- Augmented irregular pulse.
- Temperature – Normal or raised (40ºC).
- Mucous membrane – pallor, later yellow
- Dyspnoea is obvious.
- Diarrhoea; sometimes constipation.
- Mastitis.
- Gangrenous necrosis of tail, feet, pastern, ear, and teeth (occasionally).
- Milk yield reduced.
- Suffer for 2-3 days and then recumbent followed by death in a few hours /days.
If animal survives
- Weakness and Pica only during convalescence.
- There may be an additional sign of ‘P’ deficiency is recumbency.
- Affects ruminal digestion.
- Lame and bone disease
- Infertility.
- Pica.
- Fall of milk yield.
- Retarded growth and unthriftiness.
- Weakness and convalescence
- In marginal deficiency- the general condition of the herd is normal
CLINICOPATHOLOGICAL CHANGES IN NUTRITIONAL HAEMOGLOBINURIA
- Non-lactating animals of the affected herd in marginal ‘P’ deficiency area may have a normal range of inorganic P (4-7 mg %). But, lactating animals have moderately low levels of 2-3 mg. The affected animals may also have extremely low levels of 0.4 to 1.5mg.
- R.B.C decreased – Heinz body is seen.
- Urine: Dark red-brown to black, moderately turbid, No R.B.C.
- Low Cu in blood & liver.
PM changes
- Jaundiced carcass
- Blood: Dark and thin
- Swelling of the spleen
- Liver: Fatty infiltration, swollen
- Dropsy in the lower part of the body
- Discolored urine in the bladder
DIAGNOSIS AND DIFFERENTIAL DIAGNOSIS OF NUTRITIONAL HEMOGLOBINURIA IN ANIMALS
• Characteristic clinical signs like hemolytic anemia, hemoglobinuria within 4 weeks of parturition.
• Deficiency of P
Differential diagnosis
- Parasite – Babesia, Theileria
- High altitudes
- Copper Poisoning
- Plant – Rape
- Bacteria: Anthrax, Leptospira, Bacillary Haemoglobinuria
- Virus – Rinderpest
- Coldwater
- Enzootic nutritional muscular dystrophy
- Drug-induced Eg. Phenothiazine
- Enzootic haematuria
- Myoglobinuria
- Chronic hill haematuria
- Blood transfusion
- Metabolic ketosis
- Pyelonephritis
Treatment
a. Keep in a quiet and warm place.
b. Avoid laxatives and purgatives.
c. Blood Transfusion (5 to 10 liters) → followed by fluid therapy to prevent haemoglobinuric nephrosis.
c. Acid sodium phosphate 60 gm in 300 ml i/v very slow+ same dose s/c . Further s/c in at 12 hours interval for 3 times.
d. Orally drench 30 gm Sodium acid Po4 BID.
e. Copper glycinate 500mg i/v in copper deficiency causes
f. Haematinics during convalescence.
g. Bone meal 120 g BID / Dicalcium Po4.– orally for 5 days
Prevention
a. Copper gluconate 120 mg s/c.
b. Remove the cruciferous plants.
c. Adequate intake of ‘P’ during early lactation.